16 Oct, 2025
The sterilization program of the department's machine is set for 4 minutes, 5 minutes, and 6 minutes at 134°C. This chemical indicator card is labeled to monitor ranges like 2
minutes, 3 minutes, etc. Can it monitor this program?
This is a very common question, and the reasoning behind it seems logical: Is the monitoring range of this card enough? If not, does that mean it's unsafe? The next question
follows: if the program is set to maintain a few minutes at 134°C, does that mean it must be monitored by a card that changes color after the exact same time at 134°C, and
missing even one second would be unacceptable?
The answer to these questions is simple, but a bit tricky to explain: the indicator can monitor, but it’s not monitoring the program itself.
PART 1. How does the sterilization effect accumulate?
We first need to understand that a sterilization program can kill microorganisms because it continually produces a sterilization effect, much like an airplane continuously
bombing the ground. Microorganisms on the surface of the instruments are gradually killed as they continuously receive this sterilization effect.

So, how do we measure the actual sterilization effect received by the instruments?
The phrase "a few minutes at 134°C" refers only to the sterilization period (holding phase) of the sterilization process. However, for the overall sterilization effect, focusing
solely on the time at 134°C is highly inaccurate, and it actually underestimates the total sterilization effect accumulation.
Why is it inaccurate? Because there is a significant amount of sterilization effect accumulation during both the heating and cooling phases, not just during the holding phase.
Therefore, the real sterilization effect accumulation in the entire sterilization process should include the following phases: Zone 1 + Zone 2 + Zone 3.

In a moist heat sterilization environment (such as steam sterilization), the sterilization rate at 134°C is extremely high, meaning that maintaining it for about 1 minute alone can
completely kill all microorganisms (or achieve a sterility assurance level, SAL, of 10^-6).
Thus, whether it’s the ISO 17665-2 requirement of 3 minutes at 134°C or the WS 310 requirement of 4 minutes at 134°C, both are overkill programs. The only difference is who
has a higher degree of overkill. Under normal conditions, maintaining 134°C for 3 minutes will already achieve an SAL of 10^-36 or even lower, far exceeding what is required.
So, during a routine sterilization process, the actual sterilization effect applied to the instruments far exceeds the 134°C for a few minutes set for the holding phase.
PART 2. Can chemical or biological indicators monitor the program?
No, they cannot. No indicator (whether chemical or biological) can monitor whether a program has maintained a specific number of minutes at 134°C.
First, when testing the capability of chemical and biological indicators, they must be tested using a more professional, precise, and accurate instrument — a Resistometer. How
do we determine how long a chemical card changes at 134°C using the Resistometer?
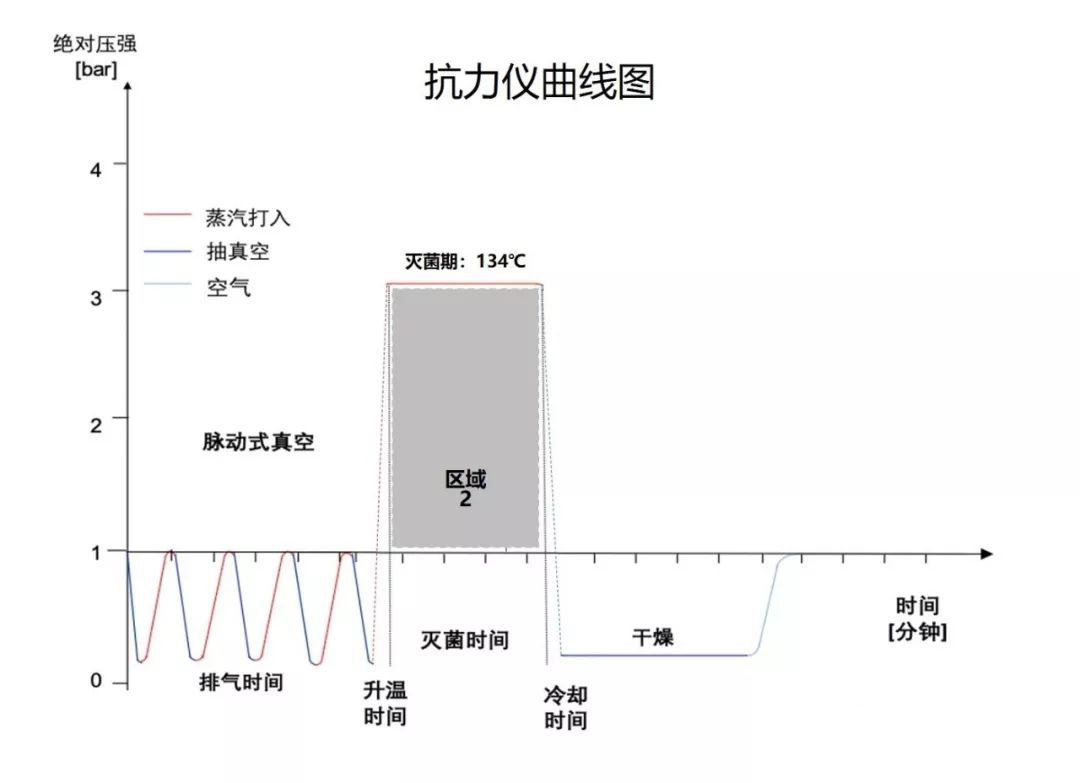
Exactly, the Resistometer will complete the heating and cooling process within 10 seconds, and the pressure rise and fall are almost instantaneous. In other words, the sterilization
effect from the heating and cooling phases is “cut out,” leaving only the sterilization effect from the holding phase (Zone 2).
Only by doing this can we get the most accurate measurement of the indicator. Therefore, as long as the sterilization effect is strong enough to kill microorganisms (or, more
precisely, more difficult to kill than the biological indicator spores), the indicator will function. Even if a card is labeled for 7 minutes at 134°C, it cannot monitor whether the medical
sterilizer has maintained 7 minutes of the holding phase, because the card is recording whether the accumulated sterilization effect is sufficient. A medical sterilizer accumulates
sterilization effects during the heating, holding, and cooling phases (Zone 1 + 2 + 3). Therefore, the card will complete its color change before the holding phase ends.
Similarly, even biological indicators, considered the "gold standard," cannot monitor the duration of the holding phase. As mentioned above, the sterilization effect at 134°C for 1
minute is enough to achieve an SAL of 10^-6 for 1 million spores. And this is considering only the sterilization effect during the holding phase, not the additional effect from the
heating and cooling phases (Zones 1 and 3). If we consider those, complete sterilization will be achieved in less than 1 minute during the holding phase in a medical sterilizer.
Thus, no indicator (chemical or biological) can truly monitor the program.
PART 3. If indicators can’t monitor the program, what are they for?
Indicators are very useful. They do not monitor the program, but whether sufficient sterilization effect (at the specific location) has accumulated.
This might sound a bit confusing, so let’s use an analogy:
Indicators don’t measure how much rain has fallen; they measure whether the ground is wet enough.
Scenario 1: Maybe only one drop of rain fell, and the ground is not wet → the indicator shows a fail;
Scenario 2: Maybe it rained moderately, and the ground is wet enough → the indicator shows a pass;
Scenario 3: Maybe it rained heavily for three days, and the ground is now a lake → the indicator shows a pass (the indicator doesn’t care how much extra rain fell).
The indicator is placed next to the instrument to “sense” whether this position received enough sterilization effect to achieve sterility. If the accumulated effect is sufficient or
insufficient, the indicator will signal a pass or fail, much like a traffic light. For an overkill program, it means the applied effect will exceed what is necessary. As long as the sterility
threshold is reached, the indicator will signal: **This location is sterile**. Any excess effect beyond this threshold is not within the indicator’s monitoring scope.
This is also why one of the requirements for Class 5 chemical indicators (which perform better than biological indicators) is that they must not change color until exposure to 135°C
for more than 1.2 minutes. This is because the sterilization effect accumulated at 135°C for 1.2 minutes (excluding the heating and cooling phases, Zones 1 and 3) is enough to kill
the most difficult microorganisms—over 100,000 spores. Therefore, as long as the set value is higher than 1.2 minutes, sterility at that location can be guaranteed.
Summary
1. Indicators (biological or chemical) are not used to monitor whether the program ran completely; they are used to monitor whether sufficient sterilization effect has been received
at the location where they are placed.
2. Indicators do not monitor how much rain fell; they monitor whether the ground is wet enough.
3. Even if a card is labeled for 7/8/9/N minutes at 134°C, it cannot monitor whether the program actually ran for 7/8/9/N minutes. Since the heating phase also contributes to the
accumulation of sterilization effects, the card will complete its color change before the set time is reached. Biological indicators will show sterilization even earlier.
Tags: